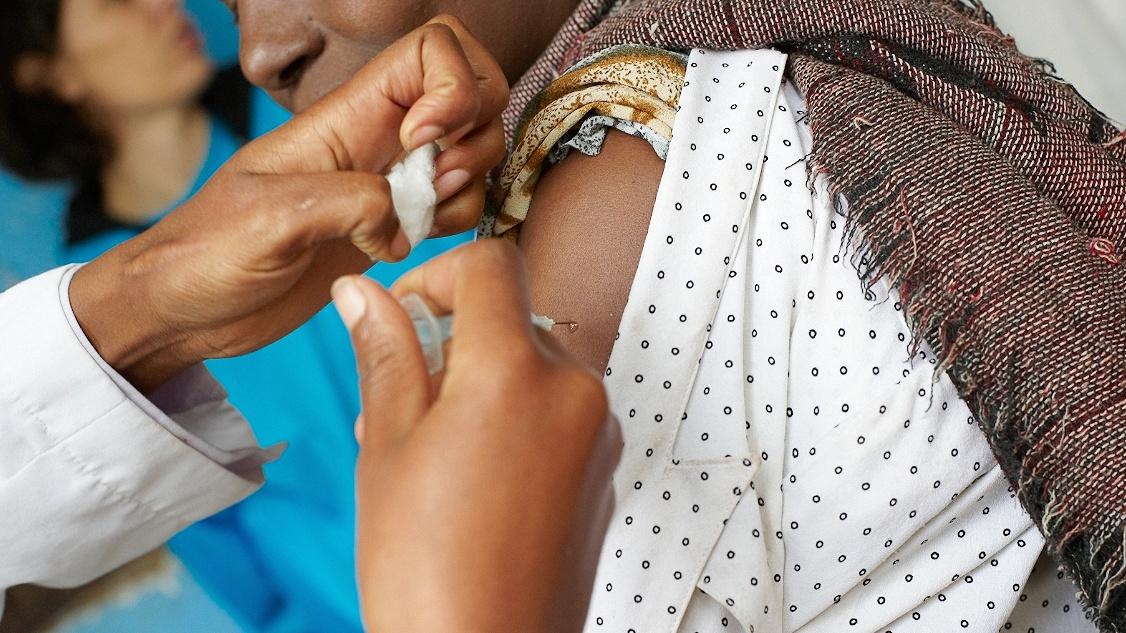
Dr Eliud Wekesa of Population Council and LSE’s Dr Ernestina Coast share their recent research in Nairobi slums where they examined the experiences of people living with HIV.
Nowhere else has been harder hit by the HIV pandemic than sub-Saharan Africa, the region alone accounts for over 68% of the total global burden. Thankfully, with introduction of anti-retroviral therapy (ART) the prognosis for people living with HIV has improved dramatically. Access to ART in low and middle income countries has expanded rapidly in recent years. In Kenya, where our study took place, 60% of those eligible are receiving ART.

Until now, research in this area has focused on access and adherence to ART. Little is known about the impact it has on people’s everyday lives, other than how effective it is as a treatment. That’s where our research is different. We wanted to know about the experiences of people living with HIV post-diagnosis, how they come to terms with their diagnosis and how they integrate it with their identity, if indeed they do. What does being HIV positive mean in the era of ART?
There are two related reasons why this kind of research is crucial. Firstly, people living with HIV have a right to sexual and reproductive health, but are they achieving this? The kinds of health services available in Kenya post-diagnosis tend to be narrowly focused on treating the biomedical disease, ignoring the psychological and social aspects that come with HIV. Secondly, we know from the evidence already available that, in certain populations, riskier sexual behaviour is increasing as knowledge grows that HIV is a manageable disease.
We interviewed residents in two Nairobi slums, aiming to characterise the experiences of people living with HIV and to explain these experiences in relation to their identity and sexuality. In our article in the BMJ Open we have focused on the narratives of three individuals, using their cases to illustrate common themes. Their biographies highlight the complex ways in which identities were transformed or maintained post-diagnosis, and how this influenced the individual’s sexual and reproductive experiences. Through their biographies we can see the ruptures that occur in the process of coming to terms with a diagnosis of HIV: from the first stage of receiving the initial diagnosis, to the disclosure of HIV status, and finally to the extent to which HIV is assimilated into a new identity.
We found services were not set up to provide the kinds of psycho-social support needed post-diagnosis in order to achieve sexual and reproductive health. Men and women living with HIV in slums are poorly served by health services post-diagnosis. There is a growing recognition of the need to support the rights of people living with HIV to be sexually active and achieve their fertility goals, while minimising HIV transmission risk. Our study is an effort in that direction.
Wekesa E, Coast E. Living with HIV postdiagnosis: a qualitative study of the experiences of Nairobi slum residents. BMJ Open 2013;3:e002399.
doi:10.1136/bmjopen-2012-002399.
This work was supported by the Wellcome Trust grant number [078471/Z/05/A].