In regions where state health systems are weak and premature death is common, it is possible for COVID-19 to have swept many parts of the world unnoticed, without the virus’ mass global awareness. Grace Akello and Julian Hopwood report from Uganda on the country’s health preparedness and quarantine measures, asking how we might measure the effectiveness of the lockdown for people’s lives and livelihoods.
This post is part of a series exploring the effects and experiences of COVID-19 prevention in Uganda.
Given our current knowledge, in the absence of medical tests COVID-19 is impossible to differentiate definitively from other illnesses: it can have no effects at all or it can kill you. Its symptoms, even the terminal ones, are not necessarily distinguishable from those of a myriad other conditions, common and otherwise. Without tests major outbreaks of the disease can still be inferred in certain contexts: in parts of Ecuador hospitals and funeral services are overwhelmed by multiple times the usual demand. What happens, though, in places where there are no funeral services and accessing healthcare is for many an unaffordable luxury? In such situations, even if the coronavirus death rates turn out to be at the high end of current estimates, it could be largely invisible. Perhaps without the massive level of global awareness it could have swept some parts of the world, including Uganda, largely unnoticed.
In these ways COVID-19 is very different to Ebola. By and large the Ebola virus is not infectious until symptoms emerge, and in around one to two weeks you are either recovering or dead. While the symptoms are not entirely unique to Ebola there is almost never any doubt from the early stages onwards that the sufferer is very, very ill. Uganda’s reputation on managing Ebola is excellent, as it is on HIV/AIDS. Our local hero here in Gulu is Dr Matthew Lukwiya who died while leading the 2000 Ebola containment efforts in northern Uganda.
A epidemic could have gone unnoticed
One question is how would anyone know whether coronavirus arrived in Uganda around 21 March 2020, when the first case was recorded, or earlier? People of all ages die here in large numbers, very often from pneumonia or unknown causes. Autopsies are extremely rare, and coroners unknown. Most people die and are buried at home, not least because hospital care is costly and hard to access for the (mainly) rural population. There are no functioning state systems for recording all deaths (and probably a majority go unrecorded), let alone causes of deaths. Families often assume that premature deaths are caused deliberately using witchcraft. Rural communities’ help-seeking behaviour can be different to that of town dwellers as costs of transport and other difficulties of accessing health services shifts the equation of what can be afforded and managed. Prolonging the lives of the elderly is not necessarily a relative priority for struggling families compared to children and income generators, a fact that is not at all inconsistent with the high level of respect in which old people are typically held.
In short, while the global awareness of coronavirus means that there is a good chance of cases being recognised in hospitals and the better community health facilities, and the slow progression of the condition may cause some people to identify it and seek treatment, this might still leave a very large proportion of COVID-19 cases and deaths unrecorded.
A massive spike in malaria cases and deaths a few years back, generated by a misconceived USAID health programme, was recognised by the Ugandan public and health services, but the weakness of official record keeping inevitably documented only a portion of the total. No one has any real idea how many additional deaths occurred, and this is for familiar, easily identified and tested malaria. According to UNICEF, over one million people die each year from malaria, and most of these are in Sub-Saharan Africa. Uganda has the highest malaria rates in the world and most are concentrated in the north, in particular Acholi, the region of about 1.5m people where Gulu is located. 10-20,000 people die each year according to official records, but this is probably an underestimate. Many of these deaths could be prevented if people were able to afford and access treatment.
The capacity for testing (and isolation)
At the time of writing (20 April 2020) 55 COVID-19 cases and no deaths have been recorded, all in people arriving from abroad (with one unexplained exception). Uganda does have a capacity to test for conditions including the coronavirus, but the problem is that it is very small in relation to need and in the past has been less than efficient. While a massive increase over the last couple of weeks in the number of tests done has been impressive – they are now doing well over 1000 each day – this is still massively less than what would be needed to give even an approximate impression of the spread (or lack of it) of the virus across the country.
In one nationally publicised case, which we have followed up, a young man, Okello, from a village deep in the countryside of northern Uganda, reported to Gulu Regional Referral Hospital complaining of a cough. It was not serious and he had only gone because he had been told to by a zealous health worker at his parish health centre following newly released Ministry of Health triage protocols.
Okello was placed in the newly commissioned Coronavirus Isolation Unit, a small dirty building that had been unused for several years with space for four beds. The Unit had been allocated a cleaner and a guard, but there was no budget or plan for care of any kind, or food. A swab had been taken on Okello’s arrival and despatched to Entebbe, with the hope that the results would come back in 48 hours. After more than a day without food, Okello was kicked out of the hut by the cleaner and, finding that the guard had gone to lunch, he took the opportunity to go home. A major man-hunt by the army ensued, with calls on the radio for Okello to be handed over to the authorities. In the meantime his results had come back negative for COVID-19. Okello was arrested, along with three of his brothers, and returned to the isolation unit, where they were told they would have to stay for a 14-day quarantine period, notwithstanding the negative result. It was made clear this was in fact a punishment for absconding rather than a more direct health measure, with possible further charges pending.
In fact, a plan had been mooted to arrest all 80 people in Okello’s village and put them in quarantine, abandoned for now for lack of both accommodation and transport (let alone a food budget). Some relatives from the village have chosen to come to Gulu, un-quarantined, to provide food for the four in the isolation hut. When questions were raised about the legitimacy of this detention, as well as the credibility that someone in a remote northern rural village might have the disease when all reported cases so far had been identified 350 km away in Entebbe in people arriving from overseas, it was announced that Okello was friends with, or maybe employed by, a Kenyan who had tested positive for COVID-19 (presumably one of the 152 cases that Kenya had then confirmed). But it was not revealed when or where they were in contact to transmit the condition. This information has been generally viewed with scepticism.
The human costs under lockdown
This government (like so many others) is in a difficult position. With an election due in 2021 they are no doubt keen to avoid a lengthy and probably extremely unpopular lockdown, enforcement of which will only draw attention to the brutality of the security forces and the extreme poverty in which so many people live. These factors and others, particularly impacts on regular health care, mean a prolonged lockdown will inevitably cost many lives.
Distribution of useful support to all those in need is probably beyond the country’s means. Any attempt to engage with the virus medically is bound to be ineffectual in the event of a major outbreak and will merely expose the chronic underfunding and sad state of health services. Mass testing and mass treatment are simply not options for reasons of cost (which might conceivably be overcome with international help) but more essentially because of a lack of human, technical and infrastructure capacity. Government medical staff have been informed that they will only be provided with masks if treating confirmed COVID-19 cases – otherwise they have to buy their own or do without. PPE is not available.
The lockdown as it stands might or might not significantly slow the progress of the disease. The chaos and corruption in the way the quarantining of overseas arrivals was carried out raises the question of whether it is already spreading pretty freely – but if so why are hospitals not seeing at least some cases? If it is not spreading, why is COVID-19 apparently behaving so very differently in East Africa to most other parts of the world? It cannot be because our lock down is more effective.
The current lockdown is now scheduled to end in early May 2020. It is possible that we will be told that COVID-19 has been successfully contained in Uganda, that the only confirmed cases are of people arriving from abroad, and that we can now get back to work. It will certainly be hard to justify it continuing if the official figures remain much as they are: 55 cases, no deaths. In the absence of much more substantial testing there will be no means of disproving these figures, and thanks to the experience of Okello and his village, people with coughs may be avoiding health services like, as they say, the plague.
How does the probably smaller effectiveness and benefit of a lockdown here (compared to richer nations) balance against the undoubtedly higher costs in lives? Is anyone working on this calculation or are the strategies we are seeing imitative, colonial inasmuch as they are imported and imposed with little consideration for local relevance or usefulness?
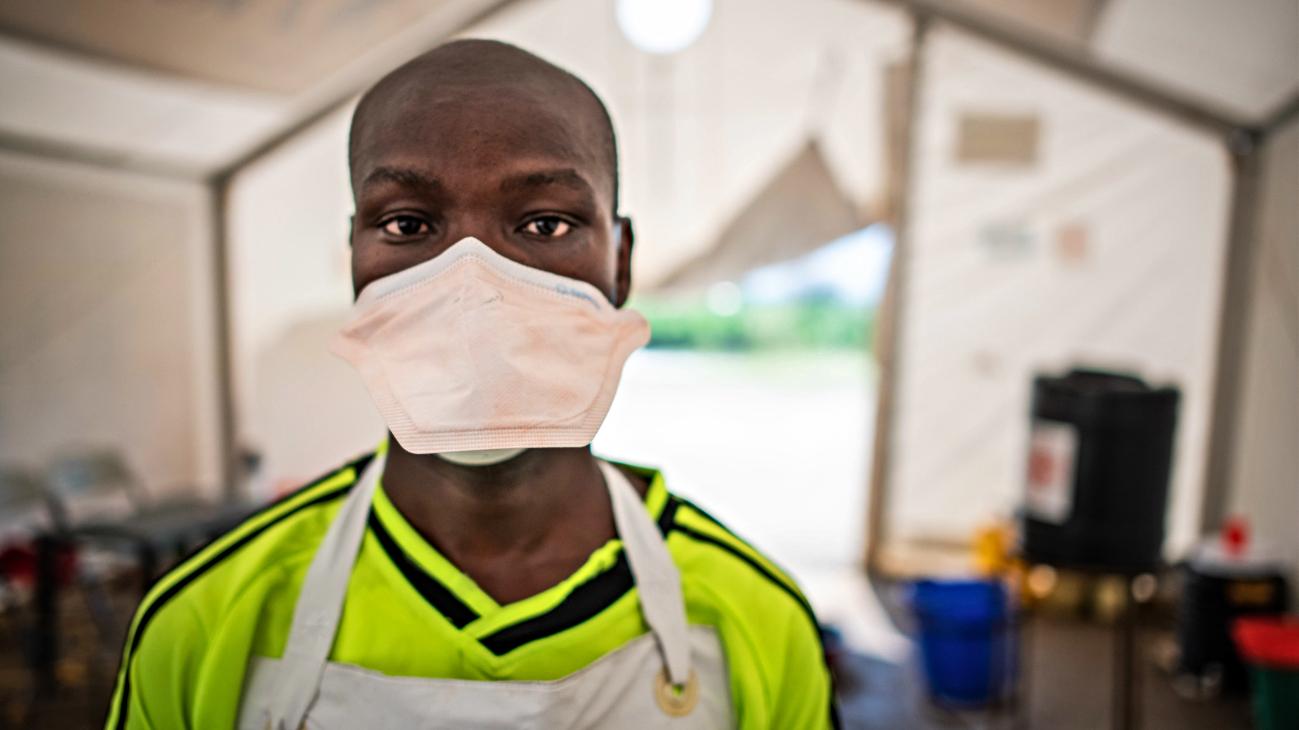
Photo: Ebola treatment unit in Grand Cape Mount, Liberia. Credit: UNMEER-Martine Perret-IOM.





You both raise many important questions relevant not only to Uganda but the whole of Africa and even the developed world.
Even in America, blacks are dying at home without a chance to see a doctor or visit a hospital. These numbers and measurements are far from accurate.
China has revised it’s numbers and now has twice as much from the original figures.
Not to mention that countries are fudging and hiding figures for political and economic motives!
It is a mess all around.
Please Keep reminding us about the pseudo measurements and sciences.
I’m almost tempted to consult the voodoo doctors-:) They might be more reliable.
I like Yahannes’ comment that “It is a mess all around” and that is an accurate statement. But I am tired of people who think that Africa is perpetually good for nothing. That is a tired story and has not taken us far, inasmuch as people have reported and reported and reported. If such reporting was adding the value that it is estimated to add, there would be nothing negative to write about Africa. It would be a so-called “high income” country by now.
This is the usual narrative about poor countries. Fortunately these poor countries are probably more resilient than the so called developed countries. Testing for COVID19 is not random, Uganda is testing based on the need and so far it has demonstrated that there is hadly community circulation. Uganda despite the poor health system has invested in containment of the pandemic because it knows that if let loose the system will not manage.
It is also absurd and misleading to say that people will die and no body will notice, even in malaria epidemics it is communities that raise an alarm so how can COVID19 kill and these communities do mot recognize the access mortality. This not rocket science. The control of COVID19 is purely behavoural no specialized services required and Africa can and will be able to surprise you.
This westren narrative should stop.
Thank you for the wonderful article; well written. Really helps understand the mindset there. In many ways they are in better shape than the USA. They started the lockdown early and are able to track the cases that enter the country. They need to remain vigilant to hold it all together. No way to get the toothpaste back into the tube once it is out. Good luck to all.
ANONYMOUS July 17, 2020
No alarming excess deaths which could be due to Covid 19 have been reported so far. We may not know for sure why. However, this report betrays a negative attitude towards the poor i.e they can’t get anything right. To underestimate the effect of the preventative measures being implemented and look for these other explanations may, sadly, be due to inherent prejudice of the Authors.
May God bless all efforts to prevent the spread of Covid 19 in Uganda, feeble and disorganised as they may appear to these authors.