In this blog, MSc student Aurore Iradukunda discusses topics covered in the LSE Department of Health Policy’s event Key policy challenges for e-Health in Africa.
Dubbed the ‘new breeding ground for global digital health’ by the Lancet in 2020, sub-Saharan Africa has welcomed a mushrooming array of digital health innovations to support its ambition towards achieving Universal Health Coverage, especially with regards to reaching rural and underserved populations. From the delivery of life-saving medical goods via drones in Rwanda, to mobile authentication services fighting counterfeit drugs in Nigeria and to robotics-powered ATM drug dispensaries in South Africa, digital health innovations hold much promise for the improvement of health services delivery on the continent. Despite the transformative potential of digital health in strengthening healthcare systems across Africa, most innovations fail to scale up as a result of unsustainable design and donor-funding, poor government ownership and coordination of pilots added to the very real challenges of fragile healthcare and digital ecosystems commonly found in sub-Saharan countries. In the webinar ‘Key policy challenges for e-health in Africa’ Mr. Nsengimana, Managing Director for Africa at the Commons Project and former Minister of Information and Communications Technology (ICT) and Youth in Rwanda, invited us to turn key policy challenges for e-health in Africa into opportunities for change.
Africa: A unique context
Mr. Nsengimana first set the scene by laying down the unique context within which digital health transformation currently operates on the continent. Firstly, with a median age of 20 years old, Africa is the continent with the youngest population in the world. There is an opportunity for African “digital natives” to accelerate and drive the adoption of technology and innovation faster than their predecessors. Secondly, with an average of 0.23 physicians per 1000 habitants and a lower than average public expenditure on health, there is an opportunity for digital health innovations to fill in the workforce and healthcare coverage gap experienced on the continent through task shifting. Thirdly, there is an opportunity to harness the increasing penetration of mobile devices seen on the continent. However, while 80.8% of Africans owned a mobile phone in 2016, Africa still has the world’s most expensive data plans with only 29.3% having access to internet and most not owning smart phones. Hybrid or internet-independent innovations such as those relying on SMS messaging have thus been preferred over Internet-based systems as the latter risk being inefficient in settings with poor internet penetration and infrastructure. Accelerating digital infrastructure and connectivity opportunities on the continent, especially in rural areas must go hand in hand with digital health transformation efforts. Lastly, while African countries share common challenges, we were reminded that Africa is not a country and that digital health transformation will and should not be a one-size fit all process on the continent.
Africa stands apart as the continent with the youngest population in the world. There is an opportunity for African digital natives to accelerate and drive the adoption of technology and innovation faster than their predecessors
e-Health Challenges in Africa: A strategy deficit problem?
When asked ‘What is the top policy challenge facing digital health in Africa?’, 40% of the audience said it related to lack of leadership and regulation. ‘‘Problems rarely have to do with bad strategies or absence of strategies. They have everything to do with implementation.’’ the former Minister of ICT and Youth tells us. In fact, according to the WHO, 42 out of 54 African countries have been reported to have a national e-Health strategy. While the growing number of e-health strategies across the continent are an indication of increased political will, their presence alone does not guarantee successful implementation. As pointed out by Mr. Nsengimana, governments must also dare to take risks through policy innovation and increased regulatory flexibility. Take the case of Zipline in Rwanda for example. The American-based drone company successfully won the scaling challenge, thanks to Rwanda quickly adapting its airspace regulations through an innovative performance-based regulatory framework making it the first country in the world to successfully implement national scale drone delivery of life-saving medical supplies. The reward of risk-taking is the opportunity to leapfrog explains the former Minister who was in office when Rwanda reached this milestone.
The 10 Ts of Digital Health Transformation in Africa
A key highlight of the webinar was Mr. Nsengimana’s ability to turn key challenges into opportunities for change through what he has coined the ‘10 Ts of Digital Health Transformation in Africa’. These are: 1) ConnecT, 2) EducaTe, 3) InnovaTe, 4) CoordinaTe, 5) InvesT, 6) PromoTe, 7) RegulaTe, 8) ProtecT, 9) TrusT and 10) QuiT. Under the ‘EducaTe’ challenge, the role of Chief Information Officers or ‘CIO’s was discussed. One can think of them as knowledge brokers at the intersection of health and technology translating the needs and concerns of stakeholders on either side. There is an imperative need for CIOs to emerge and fill up the knowledge gap between medical and tech professionals. There is also a need for digital health transformation to be demand-driven to ensure successful mass adoption of digital health innovations. While high mobile penetration on the continent can provide an enabling environment for digital health take-up, it does not necessarily translate into increased demand. This is why Digital Ambassadors programs like the one seen in Rwanda are so important to ensure mobile owners are also empowered to become digital health consumers. In fact, the Rwandan digital literacy training program follows a community-based model with the aim of catalysing the mass adoption of government-led digital initiatives such as e-government, e-health and mobile financial services.
While the growing number of e-health strategies across the continent are an indication of increased political will, their presence alone does not guarantee successful implementation. Governments must also dare taking risks through policy innovation and increased regulatory flexibility
The Future of e-Health in Africa: Further together?
To conclude, Mr. Nsengimana invited us to reflect on the future of e-health in Africa through the prism of three case scenarios developed at IntraHealth International. In the first scenario ‘Cyber Punk Africa’, described as ‘digital colonisation’, health data is harvested for profit under a system of low accountability which benefits an elite minority. Under the second scenario, termed ‘Muddling Through’, technology is routinely integrated within healthcare delivery, yet fragmentation and inequalities in care quality persist as traditional structures and roles are maintained to benefit a few. In the last and preferred scenario, ‘Further Together’, digital transformation allows for the emergence of new health partnerships and professions beyond traditional boundaries resulting in a new bold generation of leadership harnessing the benefits of technology for the greater good. What is clear is that ‘Furthering Together’ will require the deep transformation of traditional boundaries of healthcare delivery as we know them. Driving demand for e-health through an empowered consumer and entrepreneurial base will be key. Next, greater symmetrical information flow between innovators and implementers facilitated by Chief Information Officers can ensure more efficient implementation. Task shifting through the decentralisation of decision-making empowering frontline workers should be harnessed to fill the workforce gap. Digital health transformation must be nationally owned and driven. As such, new public-private partnerships in line with government priorities must be sought to ensure scalability and sustainability beyond donor support. Lastly, the benefits of technology must not be harnessed at the expense of the vulnerable or else we risk falling into traps of ‘‘healthcare as business’’ seen in many other developed economies. Governments must ensure regulatory processes ensure patient safety, equity, and data security first while at the same time embracing risk and flexibility so as to not hamper innovation. We must however be cautious of the limits of leapfrogging as digital health innovations will not be the panacea of Africa’s health challenges. The potential of e-health in Africa can only go as far as the existing health systems allow it to go and as such, can only be fully realised within resilient, integrated, sustainable, and equitable health systems.
The views expressed in this post are those of the author and in no way reflect those of the Global Health Initiative blog or the London School of Economics and Political Science.
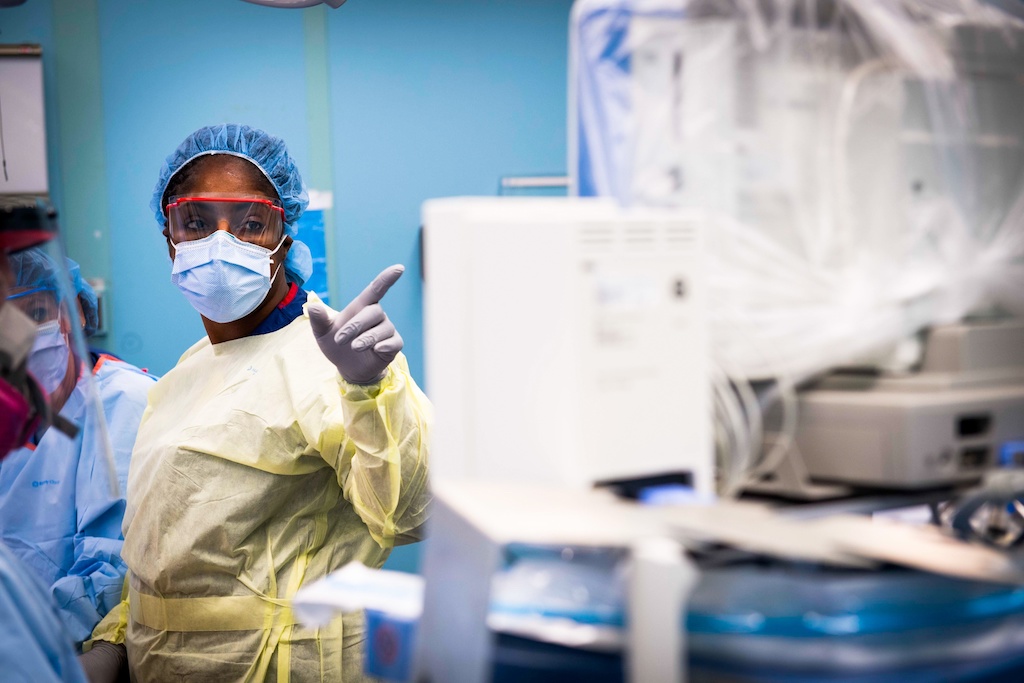
Photo by Dekeister Leopold on Unsplash




Great blog post Aurore. It does great justice to my hour-long presentation.
It was a great pleasure working with you and team @LSE on this guest lecture.
What a piece of reading! Thanks, Aurore for putting the Minister Nsengiyumva 10Ts very clear. I also like the conclusion point that ” Technology or e-health won’t be the panacea of healthcare delivery in Africa, given that much might be needed. In the health financing nomenclature, the e-health must be considered on the Strategic Purchasing Dimension. However, before getting there, there is a need to work on the other dimensions including resource mobilisation and pooling together mobilised resources. These two are as important as the strategic purchasing dimension. Thank you a lot for the clarity of your point in this blog.
Hi, nice writeup, so what are the likely challenges that could undermine digital healthcare, especially in Rwanda. Thanks
This is such an insightful piece 👏🏿
Thank you for this article. It includes helpful and relevant information.