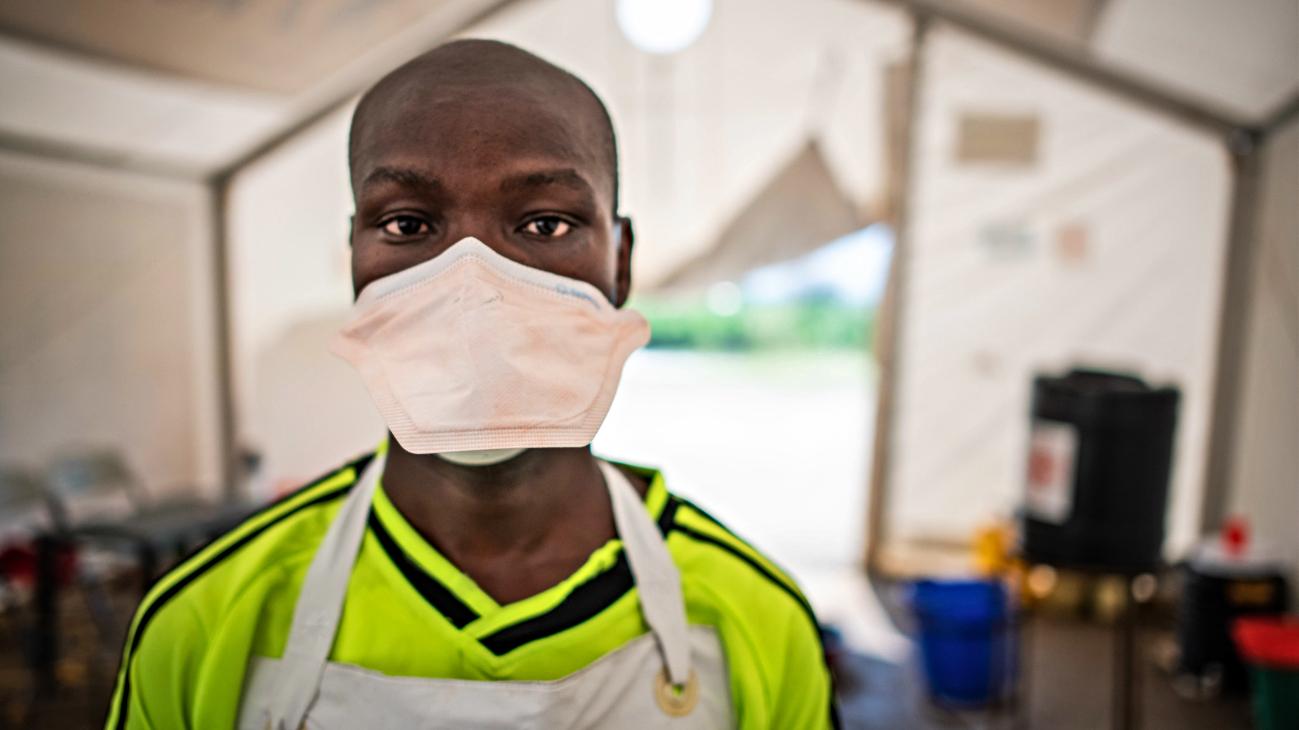
LSE’s Ernestina Coast and Emily Freeman discuss how the lack of knowledge of the Zambia’s laws on abortion means that unwanted pregnancies frequently end in unsafe procedures.
“There’s a 12 year old girl and she’s pregnant. She’s so tiny, just a small girl. She won’t be able to carry this pregnancy. What can we do doctor? We are just pitying her.”
This was the case troubling the rural health centre on the week we visited it, and the greeting of the midwife who received us. The girl, defiled by a neighbour and brought to the centre by her dad and the police, had been given a pregnancy test and sent home. The midwife was pleased to see our research collaborator, a Zambian Consultant Obstetrician-Gynaecologist. He said that if the girl could be brought to the clinic, he would review her case. An unpaid community health worker was sent to try to find her.

It was early in the morning, and outside there were queues of patients waiting to be seen at the small, 6-room facility. The midwife continued with her clinic, working alone: the centre’s other two healthcare workers had left to accompany a 17 year old girl with labour complications to a better-equipped health facility.
After the midwife had finished her clinic, we sat in her office, and she returned to the case of the pregnant 12 year old. “What can be done?” In most sub-Saharan African countries, the answer would be simple: nothing. But Zambia is different; it has one of the most liberal abortion laws in Africa. However, very few Zambians know this. This lack of knowledge means that many women and girls resort to unsafe abortion, and the overstretched health system has to deal with the consequences, which can be fatal.
After the girl was discharged following her pregnancy test, the police and health centre staff had discussed what could be done. They had no answers. Abortion was mooted, but nobody was sure about the law. Most – police and healthcare workers – had assumed that an abortion would be illegal. The girl would have to continue with the pregnancy, if her small body could cope with it.
Sitting in the midwife’s office, talking of the challenges of unsafe abortion in rural Zambia, the research team was acutely aware that somewhere in the surrounding area there was a pregnant 12 year old, and that we had knowledge of the law that might be of use to her. Time passed, and it became clear that the girl could not be found. The Consultant gave the midwife the name of a doctor at a regional hospital – 50km away by gravel road – who he knew would be able to review the girl’s case, and provide a legal abortion if that is what she wanted. He urged the midwife to ring him for any advice. Still however she seemed unsure. We asked her if she would talk to the girl and her parents about the option of abortion. She looked uncomfortable. She said she would probably only raise it if the girl’s father did. She admitted that since nobody knew safe abortion was possible, that was unlikely.
This case is not unusual. It highlights how lack of knowledge of the law – and the trained staff and facilities to support it – means that unwanted pregnancies frequently end in unsafe abortion. In rural areas this involves drinking potentially toxic herbal concoctions and inserting sticks into the uterus.
There are no data on abortion in rural Zambia. But just because there are no data does not mean that it is not a major public health issue. In September 2015 we interviewed 46 rural healthcare workers, and everyone had dealt with the consequences of unsafe abortion. Some had been approached by women trying to find out if it was possible to get an abortion, though few had been given a positive answer. Most healthcare workers assumed that abortion was illegal in Zambia, and did not know that it was possible to refer women to legal and safe abortion services. Until knowledge of the law improves, women and healthcare workers will continue to assume that abortion is illegal, and only possible using unsafe methods.
The study was carried out by Dr Ernestina Coast and Dr Emily Freeman from LSE’s Department of Social Policy along with Dr Bellington Vwalika from Zambia’s University Teaching Hospital. It was funded by the LSE’s Research Infrastructure and Investment Fund.
For more information about the study visit www.zambiatop.wordpress.com/ or follow them on Twitter @ZambiaToP
The views expressed in this post are those of the authors and in no way reflect those of the Africa at LSE blog or the London School of Economics and Political Science.