In many African countries, the existing health infrastructures struggled to meet the needs of its populations before the pandemic. Martina Nneka Onyenwe asks if the continent is prepared for the long-term effects of covid-19.
Using the past to make sense of the present
In 2020, there was a deep collective worry about the effect that covid-19 would have on the African continent. The pandemic seemed poised to undermine Africa’s fragile healthcare infrastructures. The chances of severely underfunded and critically understaffed health systems being able to absorb the predicted surge without collapse seemed slim to none.
Three years on, the reality was not nearly as catastrophic as many initially predicted. Some experts suggest that the continent’s young age demographic, temperate climate, and long-running infectious disease programmes may have contributed to most covid-19 cases being mild or asymptomatic. However, a common misconception is that mild and asymptomatic versions of covid are ‘safer’ than symptomatic cases. The after-effects of covid, regardless of the severity of the infection, may still cause significant damage to the body and create an incredible strain on a country’s health system.
It is not uncommon for viruses to trigger long-term health conditions such as autoimmune diseases, neurodegenerative disorders and cancers. It seems that SARS-CoV-2, the virus that causes covid-19, is the latest addition to that list. Those with a previous or suspected covid-19 infection are reporting higher rates of chronic heart, brain, and lung conditions compared to those who have not contracted the virus. There has been 40 million new cases of neurological disorders globally due in large part to covid infections says clinical epidemiologist Dr Al-Aly. While the percentage of people reporting such experiences is small, it is significant enough to warrant further research.
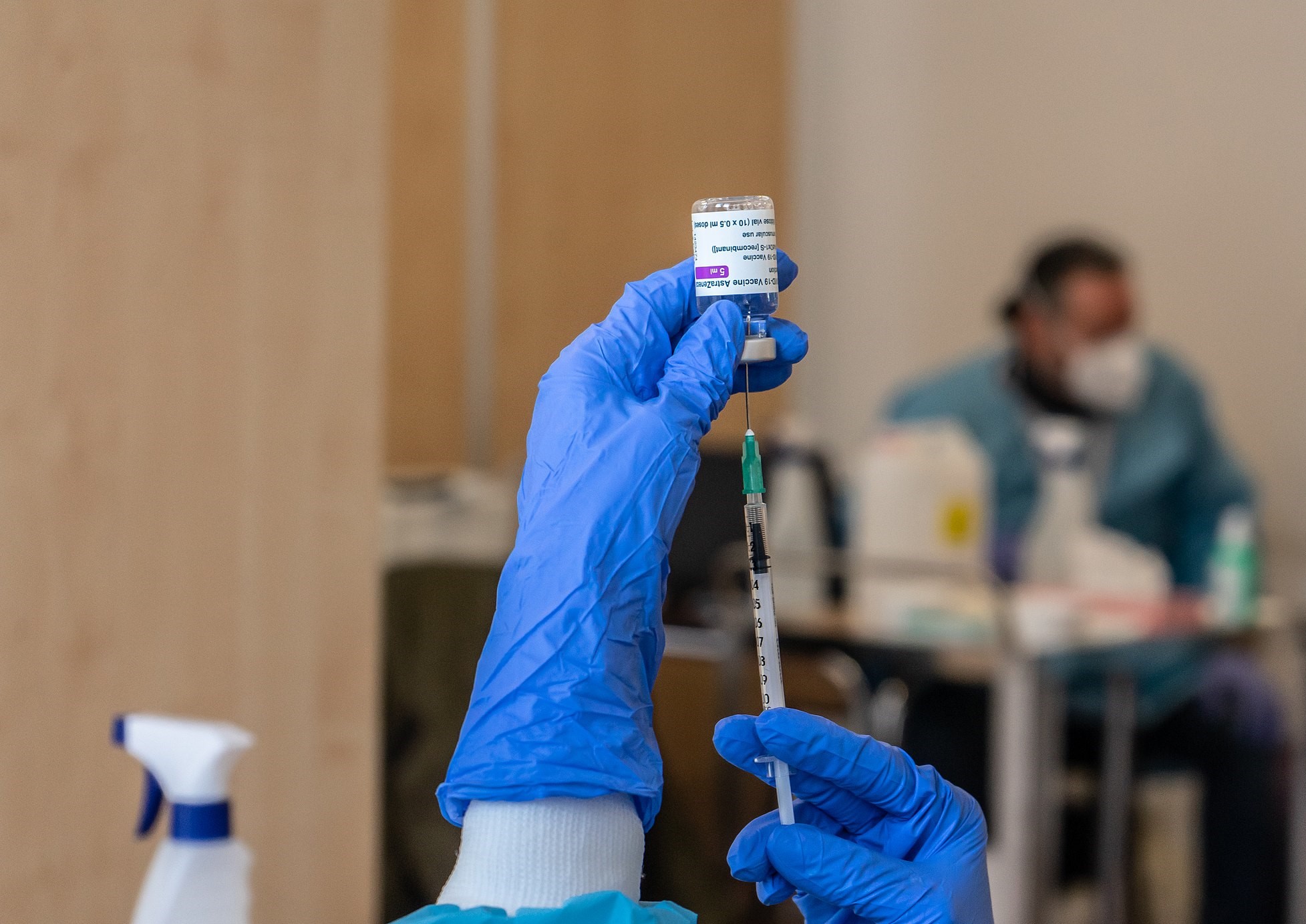
The risk of developing chronic illnesses is reduced if one is vaccinated before contracting covid. But with less than 50 per cent of the continent vaccinated, the basic protection offered by the vaccine is not being afforded to millions leaving covid-19 with the potential to noticeably increase the prevalence of chronic diseases.
Using the present to inform the future
The status quo has been undeniably disrupted. African countries can no longer simply strive to meet pre-covid targets. Although researchers are still trying to understand the extent of the damage SARS-CoV-2 does to the body, one thing has become vividly clear: the chronic diseases developed because of a mild or severe covid infection will affect the health and economic outcomes of individuals and countries.
Though this is a matter of global importance, there is reason for great concern about what this means for Africans. Particularly, that Africans will be left out of global discussions on the prevalence and impact of chronic diseases brought on by a covid infection as governments are facing major challenges in allocating resources to strengthening health systems and building healthcare worker’s technical knowledge and capacity in the face of pain points like the increased cost of living. This can translate into a data gap and reinforce the notion that since there is no proof of concern, then there is no cause for concern.
Covid-19 can trigger a chronic and extensive inflammatory response, increasing the risk of blood clots, strokes, heart attacks, liver problems and acute kidney injury. With close to 800 million confirmed cases globally, covid’s legacy of chronic illnesses will become even more apparent and encompassing in the years to come. The pandemic has heightened the need for there to be provisions to identify and treat non-communicable diseases in countries’ build back better strategies as the continent continues to navigate the pandemic’s effects.
A future informed by lessons from the past and present
Strategic solutions to covid related health challenges need to be developed with African realities in mind. One example of such holistic thinking is the bundling or integration of health services, which is currently being done in Nigeria. In August 2022, SCALES 3.0, a nationwide strategy to integrate covid-19 vaccines with routine primary healthcare services, was launched by the National Primary Healthcare Development Agency with the support of many development partners such as the Clinton Health Access Initiative. SCALES 3.0 arranges for adults to receive their covid-19 vaccine when they bring children in for routine immunisations. This is a cost-effective strategy that allows the state to use the available resources more effectively. In Imo State, Nigeria, a healthcare worker said the uptake of covid-19 vaccination has become more “encouraging” since SCALES 3.0 was rolled out.
Looking to the future, African countries may not need to invent new processes to achieve readiness against the long-term effects of covid-19. A strong recommendation is to build upon promising existing strategies and promote integration.
The effective management of covid’s long-term effects will require multiple approaches and strategies, just as the original pandemic did. By expanding interventions like the integration of primary health services to include screenings for non-communicable diseases and equipping health systems to do so there may be a chance that readiness can be achieved using already existing structures.
Photo credit: World Bank Photo Collection used with permission CC BY-NC-ND 2.0





Phenomenal article! It gave me deep insight and solid information in regards to healthcare systems in Nigeria and how covid-19 needs to be tackled and handled throughout the whole continent of Africa.
This paper was enjoyable to read, and Nigeria will undoubtedly feel the effects of Covid’s aftermath.
Incredible article! Thank you for informing us, and reminding us that the after affects of Covid doesn’t only affect American states.Knowing this information now, I hope the American government can do better and give them the vaccines and the things that Nigeria truly needs have a safer health system.
This article is well articulated and well written .In short African continent has a long way to go in terms of pandemic episodes. Love to see such a well minded young woman produce such a nice article.
This article is very informative and well written! It is imperative that we start working on tackling these issues