A number of European countries, including France, Italy, Spain, and the UK, have attempted to decentralise aspects of their healthcare systems in recent years, but what effect does this form of decentralisation have on care? Joan Costa-i-Font writes that decentralisation provides a potential mechanism for improving the equity of regional healthcare, without a significant additional cost to the public purse. However for this to occur, it is vital that decision-makers are made responsive to the demands of their citizens.
A number of European countries, including France, Italy, Spain, and the UK, have attempted to decentralise aspects of their healthcare systems in recent years, but what effect does this form of decentralisation have on care? Joan Costa-i-Font writes that decentralisation provides a potential mechanism for improving the equity of regional healthcare, without a significant additional cost to the public purse. However for this to occur, it is vital that decision-makers are made responsive to the demands of their citizens.
An increasing number of European countries, where healthcare is a publicly financed package, are exhibiting processes of political and fiscal decentralisation (e.g. Belgium, France, Italy, Spain, and the UK). The latter is not incompatible with some recentralisation in smaller states (e.g. Norway), and where healthcare has been ill-designed (e.g. Poland). Outside Europe, in the US for example, devolution of healthcare responsibilities has implied a complex operationalisation and design of federal grants to encourage state actions towards efficiency and innovation.
However, whether a health system should be centralised or decentralised largely depends on its design, and more specifically whether it incentivises efficiency, equity and quality. It all boils down to aligning political credit and fiscal blame for each policy within the health system, especially when patient mobility is limited (as is the case in Europe). Budget constraints are perceived to be hard enough on the one hand, but at the same time it requires expenditure mandates and restrictions on subnational government (e.g. as in the case of Italy and Spain with framework laws) to be kept at a minimum. In Italy and Spain, national parliaments frequently invade decentralised responsibilities, and central government frequently vetoes regional laws, which leads to conflicts of competence. Finally, equity can be ensured through equalisation grants that can take different forms and shapes.
Decentralisation is bound to fail if the central government does not decentralise the ‘blame’ of public policy action (taxation) and only decentralises mechanisms of credit claiming (expenditure). Similarly, it is bound to fail if regional governments are insufficiently funded, as it only gives rise to mounting subnational deficits. Hence, although not all decentralisation processes will result in better health system outcomes, it is possible to evaluate some of the existing evidence on expenditure trends, equity and quality to provide an informed judgment.
Effects on health expenditure
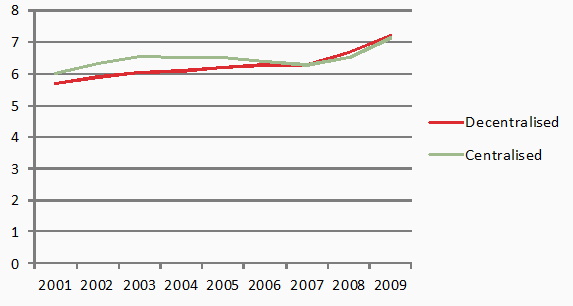
Figure 1 plots patterns of relative public health expenditure of health systems in unitary states that have or have not decentralised the provision of healthcare to subcentral governments. Importantly, evidence on unadjusted relative health expenditure suggests that decentralised health systems do not exhibit significantly different levels of relative expenditure.
Figure 1: Relative public health expenditure by healthcare constitutional form
Source: OECD, 2011
Effects on equity
A second question is that of health system equity. Figure 2 below compares regional inequalities in Spain, the UK and England. Importantly, regional inequalities in Spain, where devolution is managed regionally, have decreased by 50 per cent since 2001, while in the UK we see a more modest decline. In England, however, a highly centralised health service exhibits huge regional inequalities, more than double the level of inequality in Spain, which in turn appears stable over time.
Figure 2: Regional Inequalities (coefficient of variation of unadjusted healthcare output)

Note: The figures on the vertical axis indicate a measure of regional inequalities in healthcare – where a higher number indicates greater inequality.
Devolution in England
Greater Manchester is set to become the first English region to get full control of its health spending as part of an extension of devolved powers. This is one of the major social policy achievements of the Conservative party coalition government. Devolution provides a great opportunity to improve the accountability of the NHS, bring some innovation and take advantage of some level of policy comparison and competition. Perhaps the only criticism is that there is no assembly to ensure that the policies that the Manchester authority implements are subject to political scrutiny.
In designing a health system, it is important to keep in mind that decentralisation can bring competition by making use of the mechanisms of the political agency, which align individuals’ preferences and needs with that of their incumbents’ priorities. Evidence shows that it is possible to improve regional healthcare equity without a significant additional cost to the public purse. Nonetheless, for decentralisation mechanisms to work, political agency needs to be put in place. That is, decision-makers need to be made responsive to the demands of their constituents. It is unclear how this will take place in the English case.
Please read our comments policy before commenting.
Note: This article originally appeared at our sister site, British Politics and Policy at LSE, and gives the views of the author, not the position of EUROPP – European Politics and Policy, nor of the London School of Economics. Featured image credit: Adrian Clark (CC-BY-SA-3.0)
Shortened URL for this post: http://bit.ly/1KqOyHq
_________________________________
 Joan Costa-i-Font
Joan Costa-i-Font
Joan Costa-i-Font is an Associate Professor (Reader) in Political Economy at LSE. His research is on the economic analysis of welfare institutions, health, health care and aging, with a particular focus on Europe. He is co-editor of the Applied Economics, Perspectives and Policy (AEPP) journal.