
 How do European countries differ in helping older people choose a care home, and what is the impact of the public reporting of quality information? In a comparative study of six European countries, Ricardo Rodrigues and Andrea E. Schmidt explain that public reporting is still a far from well-established mechanism to guide the selection of care homes, and user choice often remains limited in practice.
How do European countries differ in helping older people choose a care home, and what is the impact of the public reporting of quality information? In a comparative study of six European countries, Ricardo Rodrigues and Andrea E. Schmidt explain that public reporting is still a far from well-established mechanism to guide the selection of care homes, and user choice often remains limited in practice.
In line with ageing populations across Europe, the past decade has seen a trend towards providing choice for users of long-term care and an increasing emphasis on improving quality in the sector (e.g. in England, The Netherlands and Germany). This has led to a growing reliance on market-mechanisms in long-term care, at the same time as increasing the empowerment of users to make their own choices as consumers of care. Although little evidence exists that older people’s behaviour actually corresponds to that of ‘rational consumers’, it is widely recognised that access to adequate information is essential to ensure equitable outcomes in care.

In the field of personal social services, efforts to measure and monitor quality are frequently hampered by the lack of a single acknowledged and evidence-based method for assessment, and by the multidimensional characteristics of quality, let alone the difficulties in accounting for the mix of residents and their different levels of dependency. Notwithstanding these difficulties in measurement, policy-makers and regulatory bodies in many European countries have introduced public reporting instruments in the past decade, with the intention of improving the quality of long-term care. The underlying objective is to provide consumers – i.e. older people or purchasers of care services (as e.g. in the case of care managers in England) – with enough relevant and meaningful information to guide their choices when they compare residential care homes and help them opt for the providers offering the best quality services.
We have surveyed six countries in Europe (Austria, England, Finland, Germany, The Netherlands and Spain) with distinct approaches to steering older people in their choices. In fact, in Austria, Finland and Spain efforts for quality reporting are still in their infancies, whereas The Netherlands, England and Germany have seen their well-established systems develop further in the past few years. Information on public reporting of quality in long-term care in these countries is summarised in Figure 1 below.
Figure 1: Overview of public reporting mechanisms surveyed
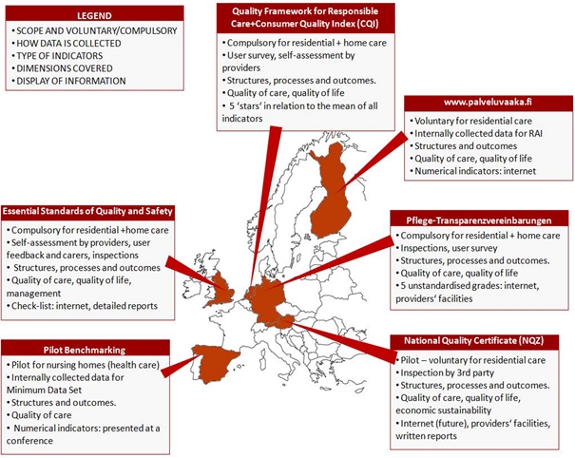
Common trends in public reporting mechanisms across Europe
The introduction of public reporting usually follows a top-down approach, with the initiative coming from regulatory bodies rather than from the industry or user groups. In the case of Austria, the Netherlands and Germany, public reporting has also served as a steering mechanism for policy-makers to bring about changes in the way quality was being assessed in the long-term care sector: e.g. by pushing for the inclusion of outcome or quality of life indicators. In all countries, however, a common understanding is emerging that quality assessment goes beyond structural indicators, and needs to take into account both process-related, and outcome indicators, such as the quality of life of older people in care homes (e.g. the Consumer Quality Index in The Netherlands).
Public reporting is more likely to be introduced, even when just as a pilot scheme, in the institutional care setting than in home care. This might have to do with particular difficulties in assessing quality in home care settings (e.g. due to the interaction with informal carers). Also, the costs of changing a care home are higher for users in residential care than when switching from one home care provider to another. Despite strong consumerist rhetoric, the introduction of public reporting mechanisms has lagged substantially behind the implementation of user choice mechanisms such as vouchers or cash benefits.
From quality management to quality improvements
As for the impact of public reporting on steering users or purchasers’ decisions, and improving quality of care, the evidence is more scarce. Evidence from the UK suggests that awareness of publicly reported indicators is fairly strong among commissioning officials (i.e. the actual purchasers of care), but much less so among users of long-term care services. In the Netherlands, there is some evidence of improved standards of quality after the introduction of public reporting, as there is in the UK, albeit it is hard to determine if these were triggered by public reporting alone. In fact, the scarce evidence base of indicators used in the Netherlands has made their use highly contested among providers of long-term care services, even leading to litigation processes taking place.
The experience of Germany and the Netherlands shows that public reporting can play a key role in increasing the profile and debate around quality assessment in long-term care. It is likely that one of the major factors for success was the application of client satisfaction surveys and the strong involvement of stakeholders at different levels in these countries.
On the whole, reporting on quality is an area that needs attention and improvement in Europe, not only in residential care but also in home care. However, some important hurdles remain for public reporting to become a driver for quality improvements. Firstly, access is often difficult for older people, especially when information is available only through the internet. Secondly, the frail cognitive condition of older people when making decisions on care, and the conditions of duress under which these decisions are often taken, may lead older people to disregard complex information on quality. Thirdly, in many countries both the (un)availability of places in care homes and strong preferences for geographical proximity when choosing a care home limit users in their actual choices. Finally, care markets are often characterised by strong barriers to entry or exit, which may diminish the effectiveness of public reporting mechanims.
Please read our comments policy before commenting.
Note: This article gives the views of the author, and not the position of EUROPP – European Politics and Policy, nor of the London School of Economics.
Shortened URL for this post: http://bit.ly/XJ2C5w
_________________________________
About the authors
 Ricardo Rodrigues – European Centre
Ricardo Rodrigues – European Centre
Ricardo Rodrigues is a Researcher at the European Centre for Social Welfare Policy and Research. His research interests include health economics, long-term care, ageing and welfare, financing long-term care and social protection systems.
_
_
 Andrea E. Schmidt – European Centre
Andrea E. Schmidt – European Centre
Andrea E. Schmidt is a Researcher at the European Centre for Social Welfare Policy and Research. Her research interests include policy choices in the design and financing of long-term care and health care systems, equity effects of social and health policies, cross-border movements of patients and providers in health care, and the successful implementation of health policies in developing countries.


