Much progress on HIV has been made – and the science has never been better – but the world lags behind in translating the advancements of science into law and policy. LSE Alum, Renu Singh argues that closing the science-policy gap is key to combatting HIV/AIDS for the purpose of bringing best practices to scale and improving health, and shows how new data from the HIV Policy Lab is helping to lead the way forward.
As the COVID-19 pandemic closes out its first year, another pandemic has been raging on for nearly four decades. Since the world discovered and isolated the human immunodeficiency virus (HIV) in the 1980s, more than 32 million people have died of AIDS-related illnesses and over 75 million people have been infected.
There has been progress over the years. The science of HIV has never been better, as the understanding of virus functionality, of the drivers of HIV infection, and of HIV testing, treatment, and prevention, have all improved. Evidence on how to use treatment as a form of prevention (e.g. pre-exposure prophylaxis (PrEP) and anti-retroviral medicines) and how to best deliver interventions (e.g. differentiated service delivery, accessible self-testing, and eliminating criminalization of key populations) have led the way forward.
Today high-quality HIV care and treatment is available in countries around the world – a remarkable story of progress from just 20 years ago, when people living with HIV in high-income countries benefited from life-saving antiretroviral drugs (ARVs) while those in low-income countries often died without such access.
But we are still far off from achieving the standard of care needed, in part because HIV-related policies and laws lag far behind the science. The world has not reached the global HIV goals set by UNAIDS for 2020, and what progress has occurred has been unequal.
On the one hand, by 2019, 14 countries had attained the global target of at least 73% of all people living with HIV achieving viral suppression. AIDS deaths were cut in half in eastern and southern Africa. On the other hand, HIV infections have increased by 72% in Eastern Europe and Central Asia, 22% in the Middle East and North Africa, and 21% in Latin America. Differences are also stark between and within countries.
Closing the science-policy gap for HIV is key to combatting the pandemic, as best practices can be brought to scale via legal action and policy to improve health and save lives. Laws and policies matter health outcomes. For instance, countries with a constitutional right to health have better health outcomes in comparison to those that do not, eliminating parental consent policies has been linked to increased rates of HIV testing, and countries that do not criminalize sex work have significantly lower HIV prevalence among sex workers.
Despite policy environments being central to HIV outcomes, there has been no convergence in countries pushing forward laws and policies that would help end the global HIV epidemic once and for all.
The HIV Policy Lab is a unique collaboration between academic, UN, and civil society organizations that aims to address this issue by bridging the gap between the science and the policy of HIV. Based at the O’Neill Institute for National and Global Health Law at Georgetown Law, the Policy Lab collects information on national HIV-related laws and policies and identifies whether, in a given year, a country has adopted each of 33 different policies that align with international standards set out by the World Health Organization, UNAIDS, international treaties, and other international authorities (see HIV Policy Lab Codebook for more information).
By providing this new data, the lab allows researchers and advocates to monitor state behavior – a critical tool in global governance – by allowing for informed comparisons among countries.
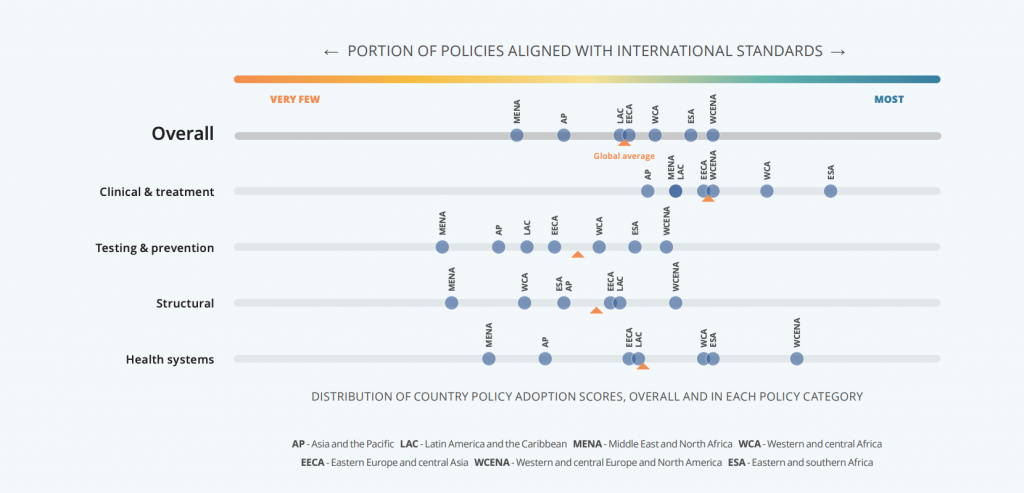
Two important takeaways emerge from this data, as described in more detail BMJ Global Health and the Policy Lab’s 2020 Global HIV Policy Report: Policy Barriers to HIV Progress. First, thus far, no country in the world has built the basic policy environment needed to combat HIV/AIDS by adopting all of the policies under investigation by the Policy Lab. Even South Africa, with the most favorable environment, has only fully adopted 27 out of the 33 policies. Of the seven UNAIDS regions, Eastern and Southern Africa, Western and Central Europe, and North America lead the world in policy progress, with overall policy adoptions scores of Many (indicating at least 60% policy adoption). However, they also exhibit significant variation across and within regions (See Figure 1).
Figure. 1. Comparing the HIV policy environments across UNAIDS regions: Regional average policy adoption scores
Second, the Policy Lab data also indicates that many of the countries and UNAIDS regions making the most progress against HIV have high policy adoption, while those with the least have policy environments not aligned with international standards. For example, the 90-90-90 targets set by UNAIDS aim to diagnose 90% of all people with HIV, provide antiretroviral therapy for 90% of those diagnosed, and achieve viral suppression for 90% of those treated, by 2020. All 14 countries that reached the 90-90-90 goal of 73% viral suppression had aligned Many or Most policies in the Policy Lab. Some of the highest policy adoption rates in the Policy Lab also came from Eastern and Southern Africa – a region that witnessed some of the most significant decline in HIV infections. Within the same region, however, South Sudan and Madagascar are seeing rising new infections, deaths in Angola have increased 36% over the last decade, and all three countries have some of the fewest policies aligned with global standards. Much work remains for the Policy Lab to untangle the complex relationship between a given policy environment and HIV outcomes, but there is good reason to believe that policy barriers are undermining the AIDS response in many countries.
As we remain engulfed in the COVID-19 pandemic, the fight against HIV offers hope. While we have multiple COVID-19 vaccines, there is still much policy work to be done to implement clinical and preventative policies, among others. More equal access to antiretroviral therapy and high-quality clinical care around the globe – thanks to advocacy, government efforts, multilateral coordination, and generous funding – shows that solidarity in pursuit of the human right to health can make a difference and saves lives. While there is still much to do to achieve this goal, we have also come a long way.
The views expressed in this post are those of the author and in no way reflect those of the International Development LSE blog or the London School of Economics and Political Science.






1 Comments