
There is ongoing discussion about how the government’s planned reorganisation will affect the NHS and therefore health inequalities. But how effective has the NHS been at reducing health inequalities in recent years? Joan Costa-Font, Cristina Hernández-Quevedo, and Alistair McGuire of LSE Health have found that while health inequalities have decreased in the past decade, often costly interventions in specific areas appear to have had little effect.
A major goal of publicly financed healthcare across the world, including the NHS, is to improve equity in the distribution of health, and in the United Kingdom health inequalities remain a top health policy priority. Interest in health inequalities began with the Black Report in 1980, which suggested occupational related differences in health were of primary importance, though policy actions to tackle health inequalities were not fully addressed until 1997.
Policies under New Labour
From 1997 onwards, policy making has explicitly targeted health inequalities and has led to the commissioning of an independent inquiry into health inequalities. The Acheson Report concluded in 1998, almost twenty years after the Black Report, that health inequalities were persistent in the UK. Subsequently the Government set a national target for health inequalities in 2000 to reduce inequalities across social classes. The aim was to reduce inequalities by 10 per cent, as measured by different health outcomes, experienced by the highest and lowest social classes, and specifically infant mortality and life expectancy at birth.
The House of Commons Health Committee has documented extensively, that although health has been improving for all, health inequalities across all common measures of health were persisting despite a range of governmental actions. A number of initiatives have been undertaken by recent governments to address health inequalities. These included the establishment of Health Action Zones (focused on preventative and wider environmental matters) in 2003. The government also outlined a cross-cutting review and a more recent initiative, introduced in 2005, aimed at tackling health inequalities in the 70 most deprived local authority areas (Spearhead areas) through targeting expenditure and policies specifically aimed at reducing these inequalities.
Have these initiatives had an impact on reducing socio-economic health inequalities?
We analysed the evolution of income related inequalities in England from 1997 to 2007. Our study used data from the Health Survey for England and measured inequalities using concentration indexes of three different health indicators, including self-assessed health (SAH), limitations in daily activities (hamp) and long-standing illness (lill). We also examined inequalities in the 70 local authority areas in England with the worst health and deprivation indicators, the so-called Spearhead areas. Examining these should tell us something about the medium term impact of policy initiatives on health inequalities.
Overall we found that socioeconomic inequalities in self-reported health and limitations in daily activities appear to be relatively constant over time, although both indicate possible decreases in the final period. We found a small decrease in inequalities in self-assessed health from 2005 through 2007, while there is a more marked increase in inequalities in this same period (2005-2007) for suffering long-standing illness. As Figure 1 shows, over the period, socioeconomic inequalities in health measured by our index fell from for self-assessed health; rose for long-term illness; and fell for daily living activities scores.
Figure 1:Socioeconomic inequalities in self-reported health in England, 1997- 2007
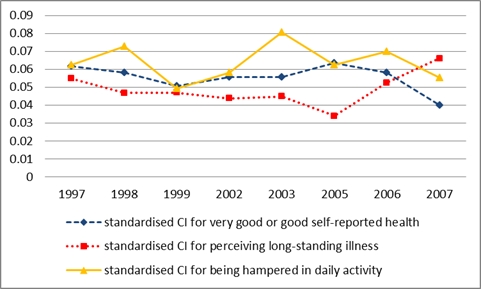
But, did any change occur in prioritised areas (Spearhead areas) as opposed to non-priority areas (that is, areas where there was no additional targeted expenditure)?
As can be seen from Figure 2, this improvement in measured inequality followed the same pattern over time for both non-Spearhead and Spearhead areas, giving no indication of effectiveness of the intervention policy. Furthermore, the deterioration in measured inequality associated with recorded long-standing illness and limitations in daily activity followed essentially the same pattern over time for both non-Spearhead and Spearhead areas, again giving no indication of effectiveness of the intervention.
Figure 2: Spearhead versus non-Spearhead area results for self-assessed health
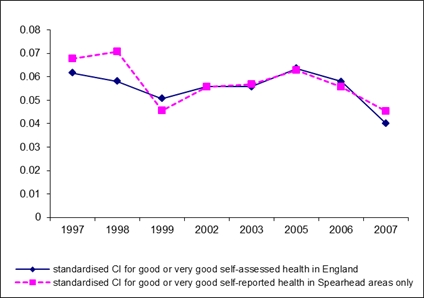
So, what can we say about the evolution of health inequalities in England?
There has been little movement in socioeconomic inequalities in health in the recent past, despite the large number of government initiatives to reduce these. There is some indication that health as measured by self-reported health may have experienced lessened income-related inequality over time. Additionally, patterns of socioeconomic inequalities in health between Spearhead and non-spearhead areas are not significantly different for any of our measured health variables.
Our results suggest that there is persistence in socioeconomic inequalities in health despite the committed resources to lessening inequalities. Specific policy interventions associated with increased targeting of health expenditure in Spearhead areas were not found to have had a short term significant impact when comparison was made to non-Spearhead areas. This confirms the suspicions of the House of Commons that not only was there no evidence on this intervention but that there was little support for the suggestion that such policies are effective
For more information, please see the longer paper Persistence despite action? Measuring the patterns of health inequality in England (1997-2007).
Please read our comments policy before commenting.





